About Osteoarthritis
What is Osteoarthritis?
Osteoarthritis (OA) is the most common type of arthritis, also known as degenerative joint disease, for which there is no cure. It is a common, chronic, progressive musculoskeletal disorder.
In an osteoarthritic joint, the surface layer of cartilage gradually breaks down and wears away. The bones in the joint that are now exposed and rubbing against each other, causing pain, swelling, and loss of motion. Over time, the joint may lose its normal shape. In addition, small deposits of bone, called bone spurs, may grow on the edges of the joint. These can break off and float inside the joint space, causing even more pain and damage.
80% of the population over 65 years old has radiographic evidence of OA.1 Patients suffering from OA often face chronic pain that worsens over time. Most commonly affecting middle-aged and older people, OA can range from very mild to very severe. There are certain factors that can increase a person’s risk for developing osteoarthritis.
CAUSES OF OSTEOARTHRITIS
- Aging: as a person gets older, the body’s ability to heal damaged or lost cartilage decreases2
- Joint injury: younger people can also develop OA due to joint injury, for example, athletes who have suffered from a sports-related knee injury3
- Heredity: if there is a family history of OA, the risk for developing the disease increases4
- Repeated joint stress: excess weight or overuse of the joint causes stress or increased wear and tear on the joint2
- Muscle weakness: if the muscles that surround the joint are weak, added stress is placed on the joint5
- Joint disorder: if there is a joint malformation or a genetic defect in the joint cartilage
JOINTS THAT CAN BE AFFECTED BY OA
Osteoarthritis is the most prevalent joint disorder worldwide and is associated with significant pain and disability.6 It is a progressive disease that can affect any joint but most often involves the weight bearing joints.
Joints that can be affected include:
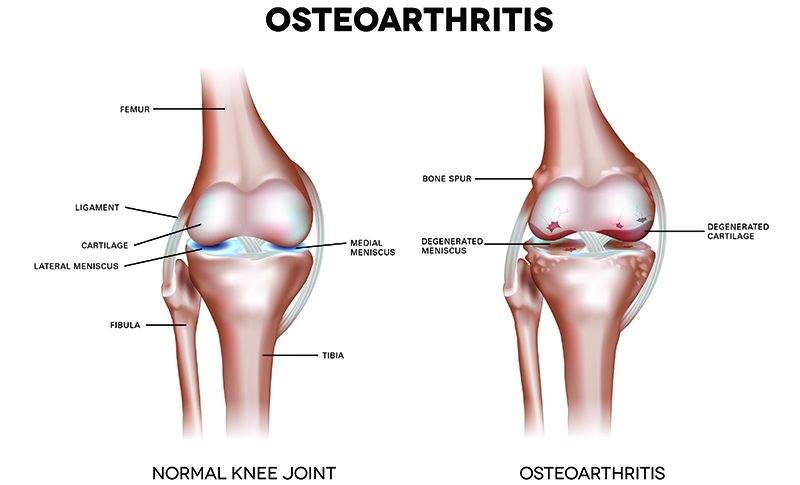
A significant proportion of the world’s population is afflicted by OA of the knee, and the disease ranks as either the top or second leading cause of disability.7
SYMPTOMS OF OA
- Pain
- Swelling
- Stiffness
- Limitation or loss of physical function
- A crackling sound when moving the joint
THINK YOU HAVE OA?
Living with osteoarthritis can not only be painful, but also discouraging. Osteoarthritis is the most common cause of knee pain. Patients who think they may have OA should talk to their doctor. Although there is no cure for the disease, the sooner patients start treatment, the more manageable their OA may become, and the longer they may be able to delay surgery or total knee replacement.
1. Loeser, R., MD. Age-Related Changes in the Musculoskeletal System and the Development of Osteoarthritis. Clin Geriatr Med. 2010 Aug; 26(3): 371–386. doi: 10.1016/j.cger.2010.03.002.
2. Markenson, J., MD. An In-Depth Overview of Osteoarthritis. Hospital for Special Surgery. Web: https://www.hss.edu/conditions_an-in-depth-overview-of-osteoarthritis.asp
3. Guccione, A.A., et al., The effects of specific medical conditions on the functional limitations of elders in the Framingham Study. American journal of public health, 1994. 84(3): p. 351-8.